Introduction
Epidemiological evidence supports a strong positive relationship between bioavailable estrogen and bone mass in both women and men (
Khosla et al. 2001;
Piot et al. 2019). Estrogen actions are mediated in part by estrogen binding to the estrogen receptor (ER), which is found in two isoforms, ERα and ERβ. Both ERα and ERβ are found in bone; however, ERα is more prevalent in cortical bone, whereas ERβ is more widely distributed in cancellous bone (
Onoe et al. 1997). ERα and ERβ knockout mouse models have been used to determine the significance of this differential expression in the growth and maintenance of bone mass. Male ERα knockout (ERKO) mice generally show increased cancellous bone but decreased cortical bone mass, whereas male ERβ knockout mice show equivalent bone mass when compared with wild-type (WT) mice (
Vico and Vanacker 2010). However, total bone mass is only one determinant of bone strength (
Ammann and Rizzoli 2003;
Fonseca et al. 2014), and reduction in estrogen signaling can affect all levels of bone’s hierarchal structure (
Khosla et al. 2012;
Khalid and Krum 2016), which collectively determine fracture resistance.
Ultimately, the three-dimensional structure of bone is controlled via activity of osteoblasts, osteoclasts, and osteocytes. Osteocytes express sclerostin, a protein that down-regulates bone formation by inhibition of Wnt signaling (
Delgado-Calle et al. 2017) through paracrine actions on local osteoblasts and osteoclasts (
Robling et al. 2008;
Moustafa et al. 2012). Sclerostin expression is regulated by several external factors such as age and mechanical loading as well as endogenous hormones such as IGF-I, parathyroid hormone, androgens, and estrogens (
Delgado-Calle et al. 2017). In women and female rodent models, estrogen status is inversely related to sclerostin expression, whether measured via serum sclerostin concentrations (
Mirza et al. 2010;
Mödder et al. 2011a;
Kim et al. 2015a) or sclerostin mRNA or protein expression in the bone (
Kim et al. 2012;
Fujita et al. 2014;
Jia et al. 2014). In men, circulating sclerostin is negatively correlated with testosterone concentrations (
Di Nisio et al. 2015), though correlation does not prove direct regulation. In fact, estrogen treatment of elderly men decreased circulating sclerostin, whereas testosterone treatment did not (
Mödder et al. 2011b). This implies that estrogen directly regulates circulating sclerostin in men, though the direct impact on bony sclerostin and whether this regulatory role requires ERα is still unknown. Thus, further studies looking at the effect of estrogen on bone sclerostin expression in males are warranted.
In this study, we compare aged male ERKO mice with their age-matched WT counterparts. We hypothesized that aged male ERKO mice would have improved trabecular microarchitecture in both the femur and the lumbar vertebrae, as well as decreased femoral length, mineral content, and cortical bone area compared with WT mice. Additionally, we hypothesized that, versus WT, male ERKO mice would have a higher percentage of sclerostin-positive (Sost+) osteocytes in cortical bone.
Results
Metabolic characteristics
The metabolic characteristics for these animals have been previously published as part of a larger study (
Winn et al. 2018) and the results have been summarized in
Table 1. Briefly, ERKO mice had higher body fat percentage (
p = 0.026), fasting glucose (
p = 0.024) and triglycerides (
p = 0.013) compared with WT mice. No differences were detected between groups in body weight, absolute food intake, circulating estradiol, or fasting levels of insulin, total cholesterol, high-density lipoprotein, low-density lipoprotein, or nonesterified fatty acids.
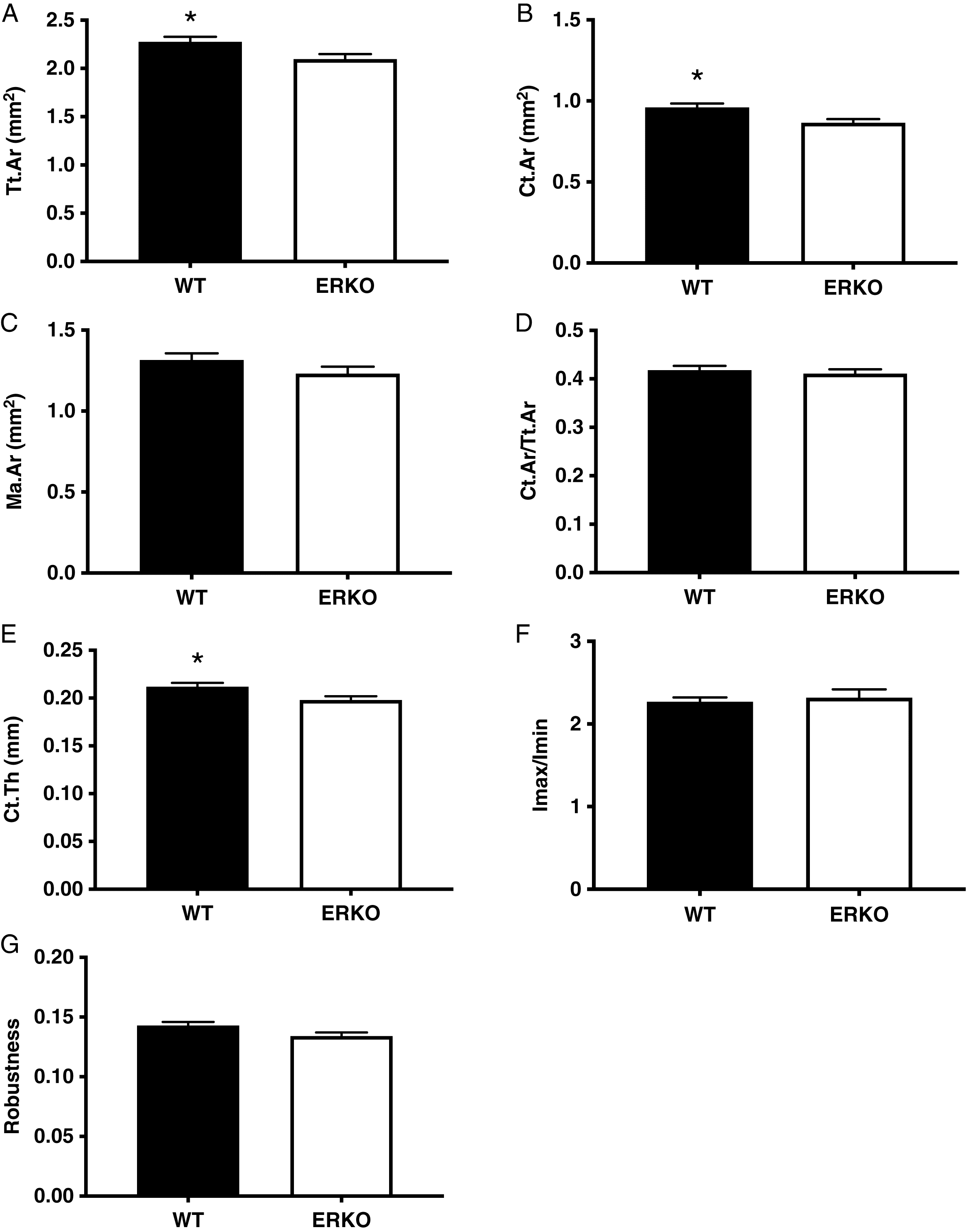
Femoral cortical geometry
Femur length was not different between WT and ERKO animals (WT: 15.80 ± 0.17 mm and ERKO: 15.73 ± 0.17 mm;
p = 0.788), though there was a trend toward an increase in robustness in the WT group over the ERKO animals (WT: 0.143 ± 0.003 mm and ERKO: 0.134 ± 0.003 mm;
p = 0.075). ERKO mice showed significantly lower Tt.Ar (ERKO: 2.096 ± 0.052 mm
2 and WT: 2.277 ± 0.052 mm
2;
p = 0.042), Ct.Ar (ERKO: 0.865 ± 0.023 mm
2 and WT: 0.961 ± 0.023 mm
2;
p = 0.018), and Ct.Th (ERKO: 0.198 ± 0.004 mm and WT: 0.212 ± 0.004 mm;
p = 0.047) compared with WT animals. There were no differences between groups in Ma.Ar (WT: 1.315 ± 0.042 mm
2 and ERKO: 1.232 ± 0.042 mm
2;
p = 0.205) or Ct.Ar/Tt.Ar (WT: 0.418 ± 0.009 and ERKO: 0.411 ± 0.009;
p = 0.629). No differences were seen in the Imax/Imin ratio, a measure of the circularity of the diaphysis (
Shaw and Stock 2009), between groups (WT: 2.287 ± 0.113 and ERKO: 2.364 ± 0.113;
p = 0.655) (
Fig. 1).
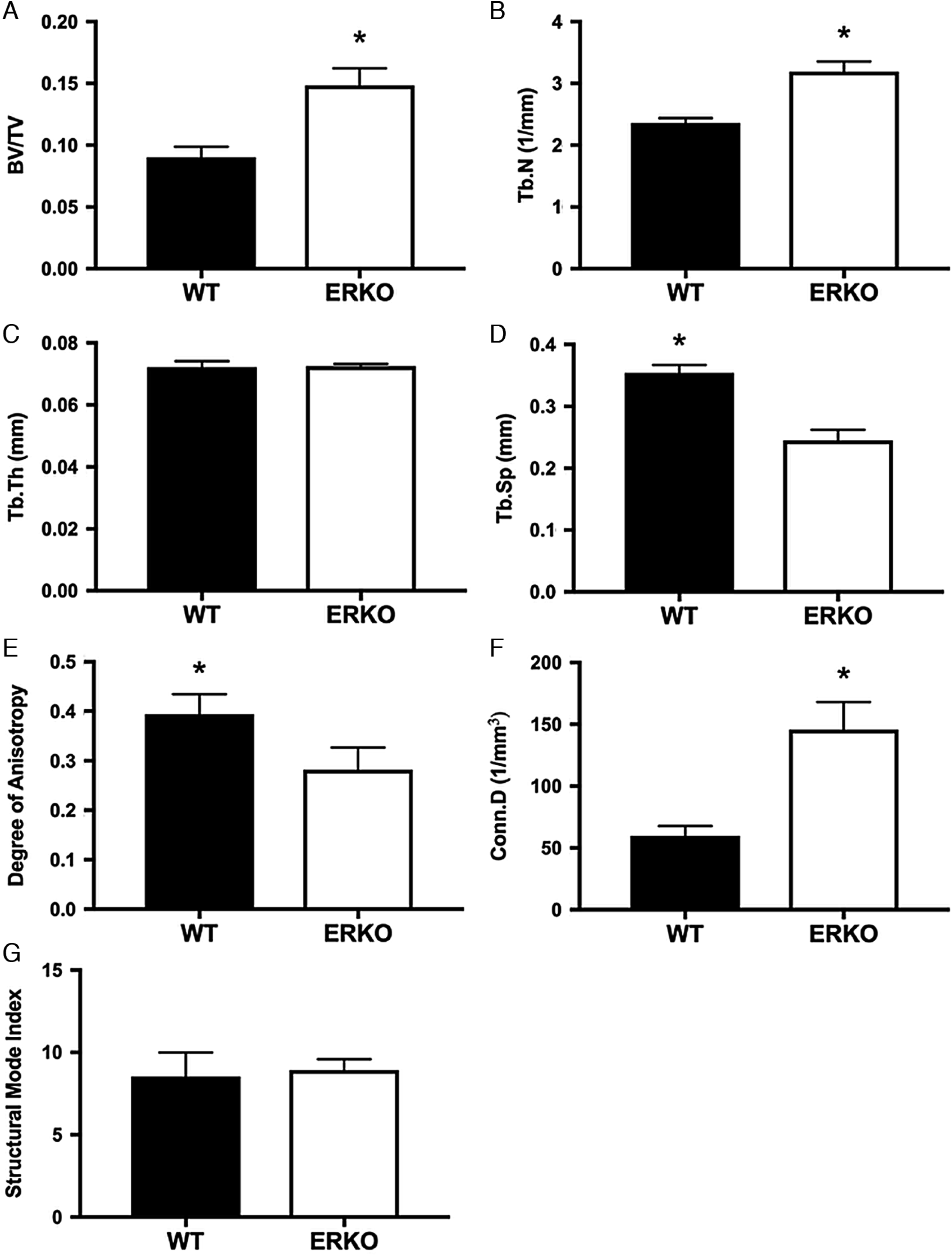
Femoral trabecular microarchitecture
ERKO mice had significantly higher BV/TV (ERKO: 0.149 ± 0.011 and WT: 0.090 ± 0.011;
p = 0.002), Tb.N (ERKO: 3.192 ± 0.128 mm
−1 and WT: 2.360 ± 0.128 mm
−1;
p = 0.001), and Conn.D (ERKO: 145.69 ± 16.76 mm
−3 and WT: 59.76 ± 16.76 mm
−3;
p = 0.005), compared with WT animals. ERKO mice had significantly lower Tb.Sp (ERKO: 0.245 ± 0.015 mm and WT: 0.354 ± 0.015 mm;
p = 0.001) and DA (ERKO: 0.263 ± 0.029 and WT: 0.373 ± 0.027;
p = 0.021) compared with WT animals. Tb.Th (ERKO: 0.073 ± 0.001 mm and WT: 0.072 ± 0.001 mm;
p = 0.875) and SMI (ERKO: 8.927 ± 1.120 and WT: 8.548 ± 1.120;
p = 0.816) were not different between groups (
Fig. 2).
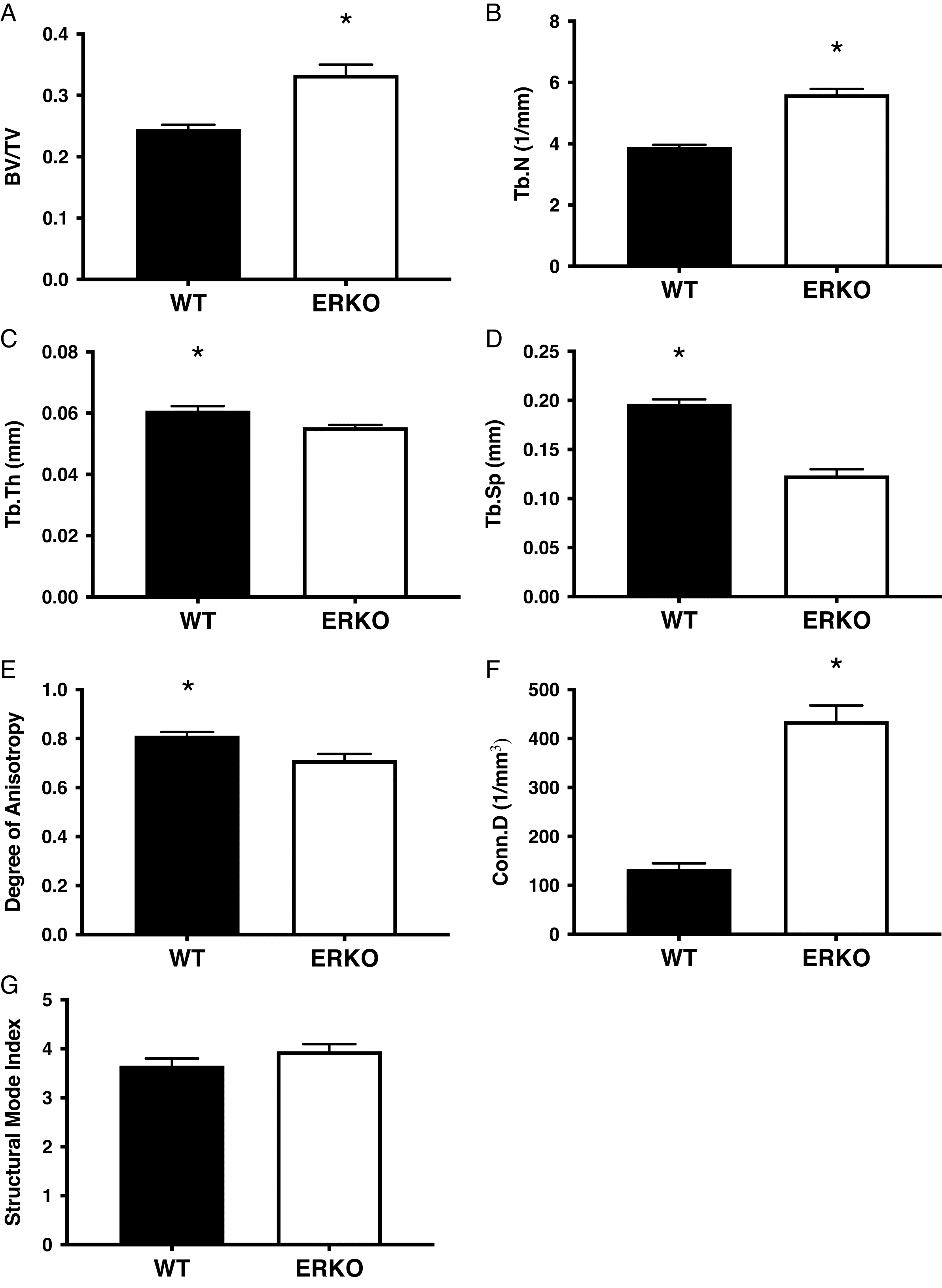
Vertebral trabecular microarchitecture
ERKO mice had significantly higher BV/TV (ERKO: 0.334 ± 0.013 and WT: 0.245 ± 0.013;
p = 0.001), Tb.N. (ERKO: 5.616 ± 0.137 mm
−1 and WT: 3.891 ± 0.137 mm
−1;
p = 0.001), and Conn.D (ERKO: 435.42 ± 24.28 mm
−3 and KO: 133.36 ± 24.28 mm
−3;
p = 0.001) compared with WT mice. ERKO mice had significantly lower Tb.Th (ERKO: 0.055 ± 0.001 mm and WT: 0.061 ± 0.001 mm;
p = 0.008), Tb.Sp. (ERKO: 0.124 ± 0.005 mm and WT: 0.197 ± 0.005;
p = 0.001), and DA (ERKO: 0.713 ± 0.021 and WT: 0.812 ± 0.021;
p = 0.007) compared with WT mice. There was no significant difference in SMI (ERKO: 3.946 ± 0.146 and WT: 3.656 ± 0.146;
p = 0.187) between groups (
Figs. 3 and
4).
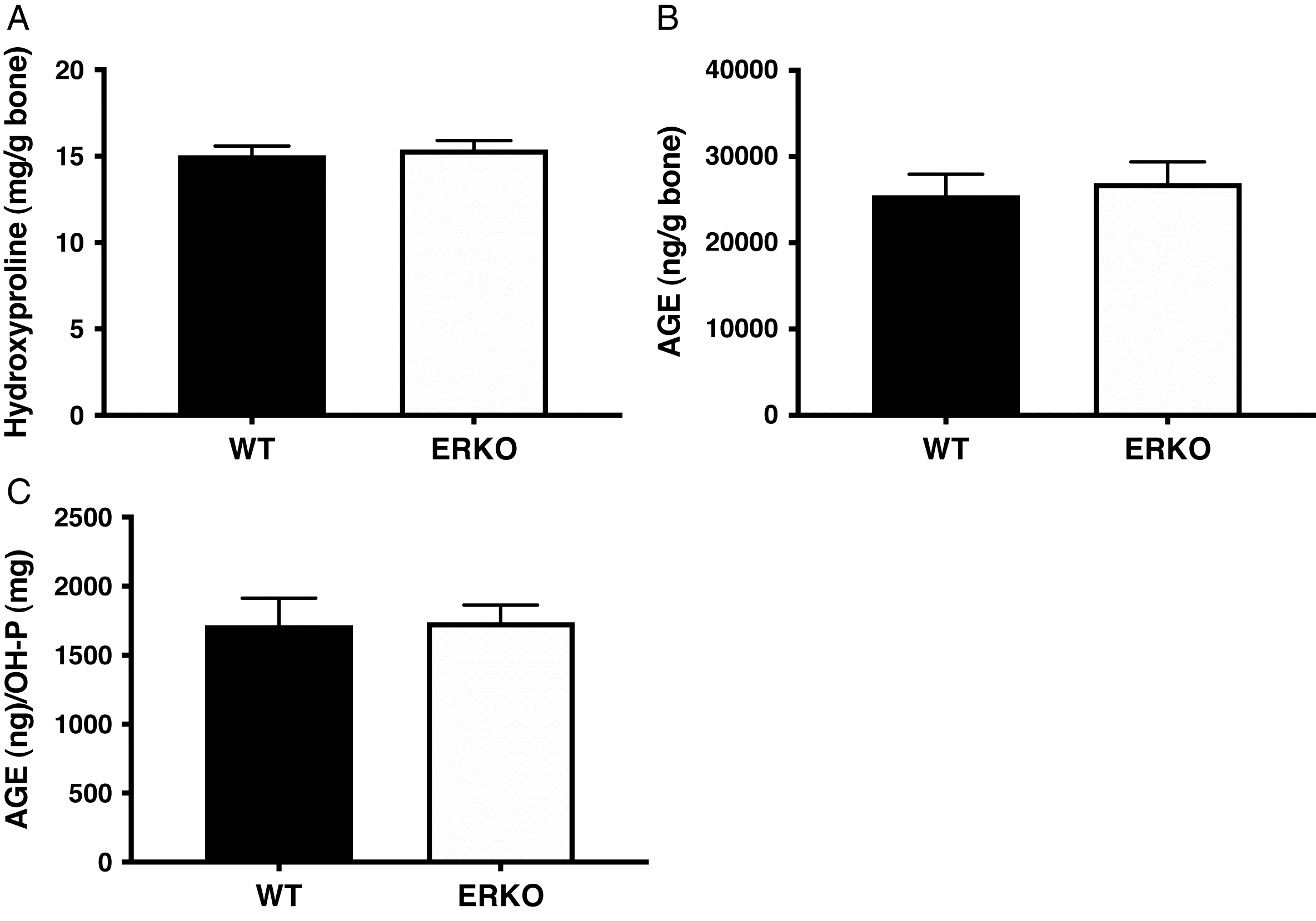
Femoral cortical collagen and AGE content
No differences were seen in total femoral collagen content (mg hydroxyproline/g bone) between groups (WT: 15.05 ± 1.32 and ERKO: 15.39 ± 1.34;
p = 0.654). There were no differences in total femoral AGE content (ng quinine/mg bone) between groups (WT: 25.53 ± 5.93 and ERKO: 26.92 ± 6.49;
p = 0.697). Relative to total collagen content, there also were no differences in AGE content (ng quinine/mg hydroxyproline) between groups (WT: 1718.1 ± 477.6 and ERKO: 1739.0 ± 332.3;
p = 0.928) (
Fig. 5).
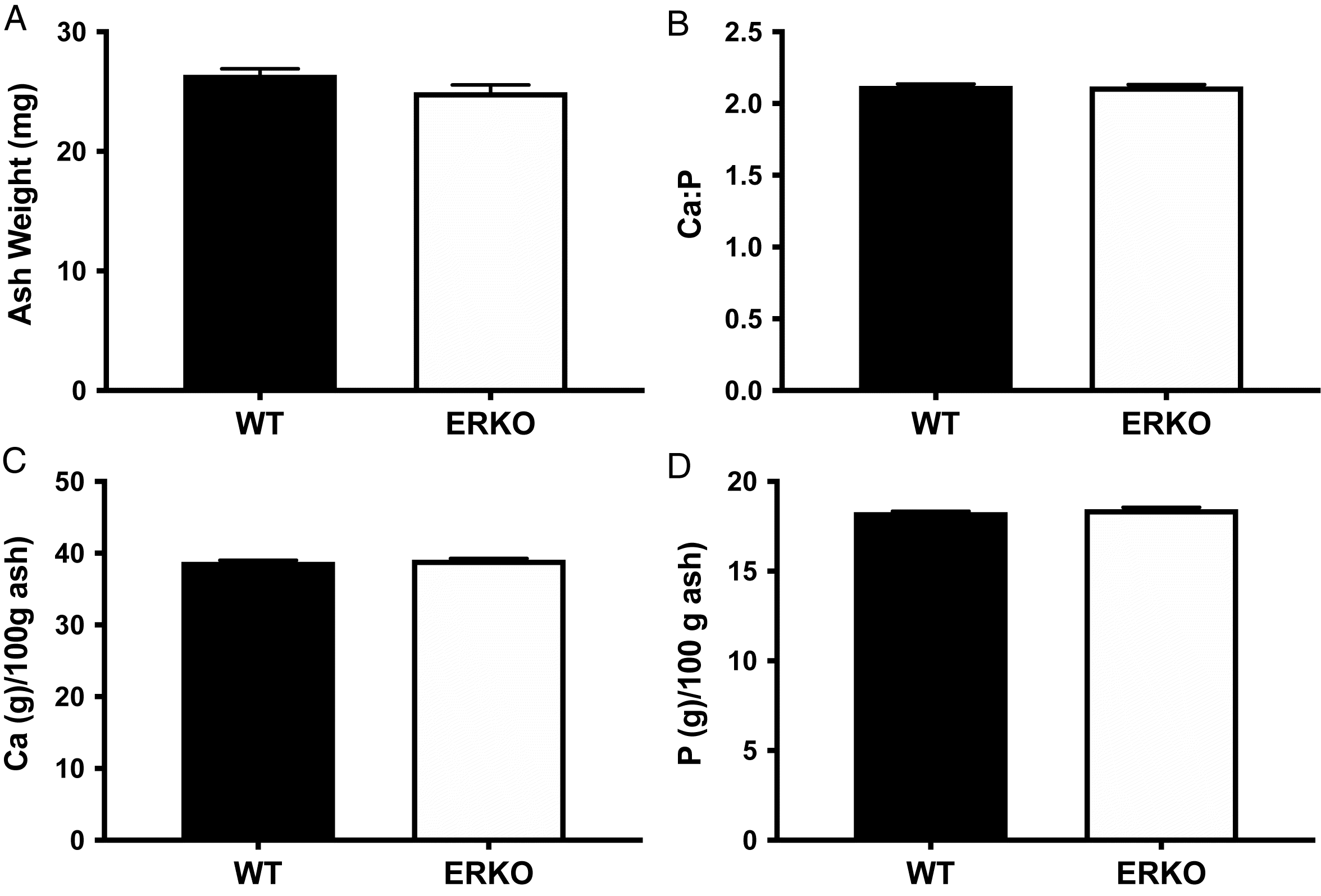
Ash and mineral content
There were no differences in total ash weight between groups (WT: 26.42 ± 0.55 mg and ERKO 24.97 + 0.55 mg;
p = 0.092). No differences in calcium content (g Ca/100 g ash) were detected between groups (WT: 38.83 ± 0.45 and ERKO: 39.11 ± 0.42;
p = 0.286). There were no differences in phosphorus content (g P/100 g ash; WT: 18.26 ± 0.14 and ERKO: 18.46 ± 0.26;
p = 0.181) or the calcium to phosphorus ratio between groups (WT: 2.12 ± 0.03 and ERKO: 2.12 ± 0.03;
p = 0.834) (
Fig. 6).
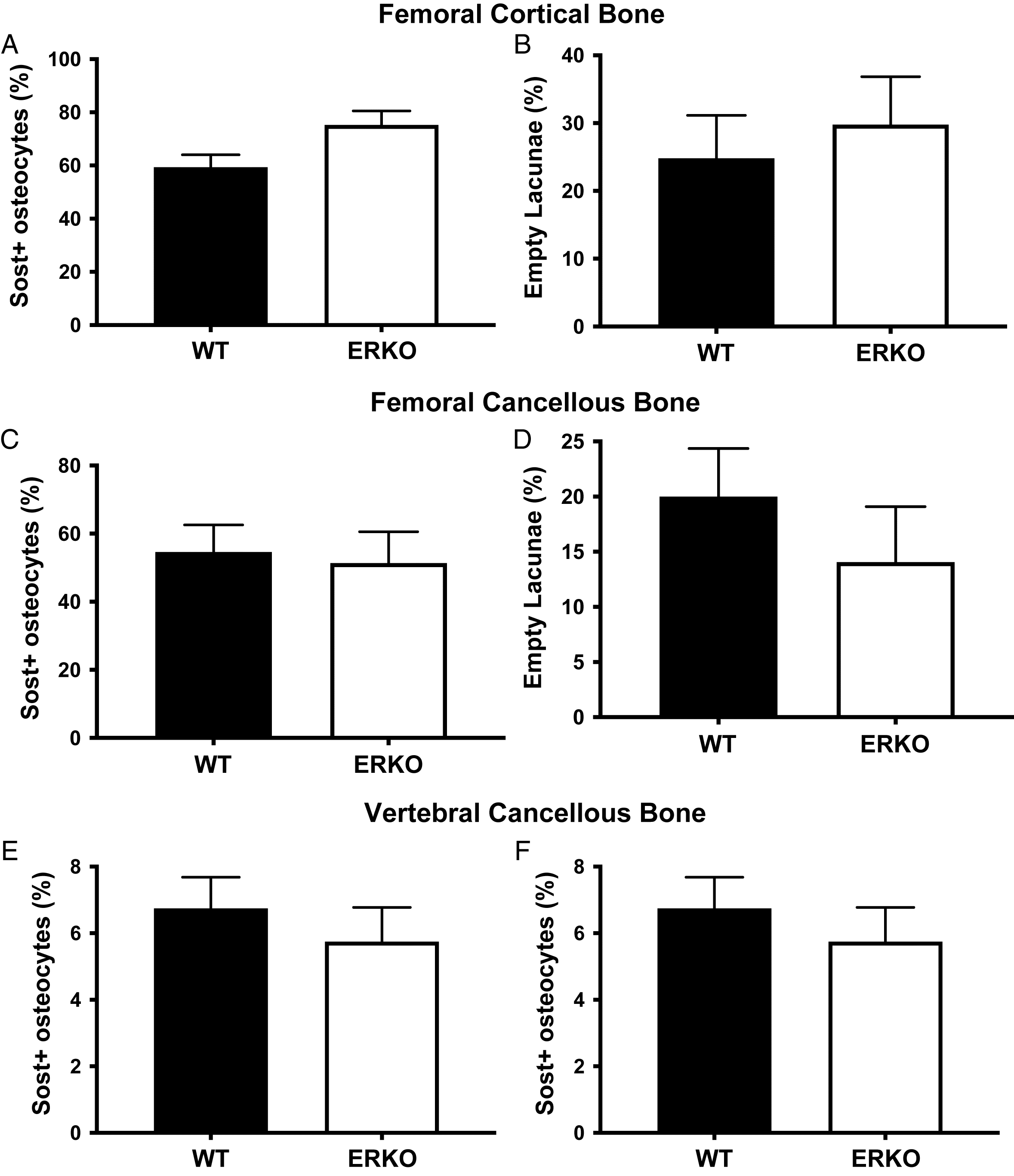
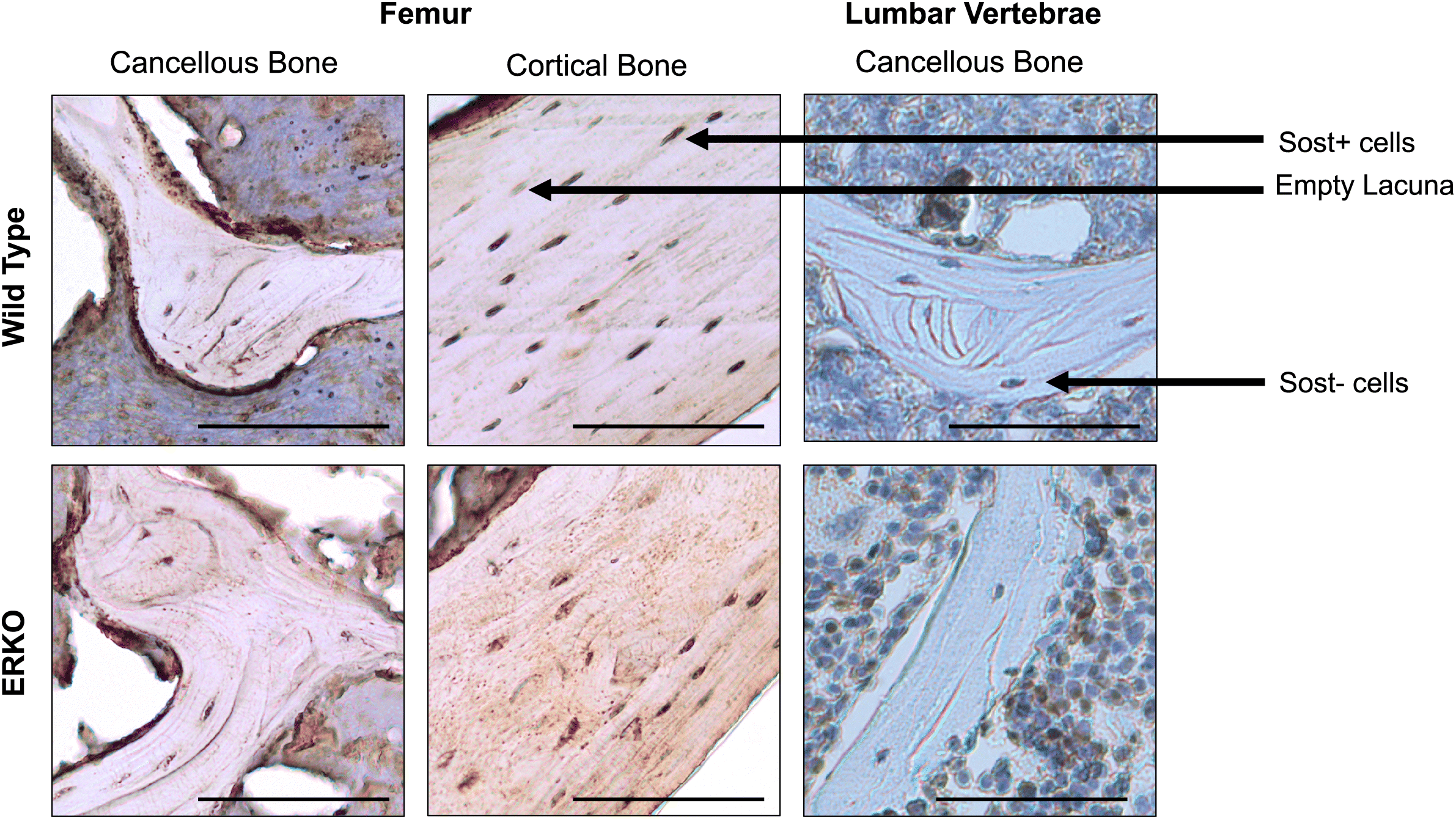
Osteocyte sclerostin expression
There was a trend towards an increase in percentage of Sost+ osteocytes in ERKO animals compared with WT (WT: 59.35% ± 4.69% and ERKO: 75.30% ± 5.25%;
p = 0.058) in the cortical bone of the femoral diaphysis, but there were no differences in cancellous bone of the femoral metaphysis (WT: 54.61% ± 7.93% and ERKO: 51.39% ± 9.15%;
p = 0.801) or the lumbar vertebrae (WT: 6.75% ± 0.94% and ERKO: 5.75% ± 1.03%;
p = 0.491). No differences were detected in percentage of empty lacunae between WT and ERKO animals in cortical bone of the femoral diaphysis (WT: 24.82% ± 6.32% and ERKO: 29.79% ± 7.07%;
p = 0.617), or cancellous bone of the femoral metaphysis (WT: 20.01% ± 4.35% and ERKO: 14.07% ± 5.03%;
p = 0.413), or the lumbar vertebrae (WT: 13.31% ± 2.85% and ERKO: 20.55% ± 3.12%;
p = 0.119) (
Figs. 7 and
8).
Metabolic influences on skeletal outcomes
Since ERKO can alter metabolic function, and metabolic health can have significant impact on the skeletal phenotype, we determined whether impaired metabolic health was associated with any skeletal outcomes. There were significant positive correlations between circulating fasting glucose and BV/TV of the femoral distal metaphysis (r = 0.666, p = 0.018), Tb.N (r = 0.670, p = 0.017), and Conn.D (r = 0.623, p = 0.031). There were significant negative correlations between circulating fasting glucose and Tb.Sp (r = −0.668, p = 0.018) and DA (r = −0.634, p = 0.036) of the femoral distal metaphysis. In the lumbar vertebrae, there were significant positive correlations between fasting glucose and BV/TV (r = 0.672, p = 0.017) and Tb.N (r = 0.594, p = 0.042), and a significant negative correlation between fasting glucose and Tb.Sp. (r = −0.622, p = 0.031).
We tested trabecular outcomes with fasting glucose as a covariate to assess the influence of circulating glucose on the group differences seen. In the femoral distal metaphysis, significant differences between groups remained in Tb.N (without glucose: ERKO: 3.192 ± 0.128 mm−1 and WT: 2.360 ± 0.128 mm−1, p = 0.001; with glucose: ERKO: 3.111 ± 0.143 mm−1 and WT 2.441 ± 0.143 mm−1, p = 0.015) and Tb.Sp (without glucose: ERKO: 0.245 ± 0.015 mm and WT: 0.354 ± 0.015 mm, p = 0.001; with glucose: ERKO: 0.254 ± 0.017 and WT: 0.345 ± 0.017, p = 0.008) when glucose was included as a covariate. Significant group differences (KO vs. WT) changed to trending group differences in BV/TV (without glucose: ERKO: 0.149 ± 0.011 and WT: 0.090 ± 0.011, p = 0.002; with glucose: ERKO: 0.142 ± 0.013 and WT: 0.097 ± 0.013, p = 0.056) and Conn.D (without glucose: ERKO: 145.69 ± 16.76 mm−3 and WT: 59.76 ± 16.76 mm−3, p = 0.005; with glucose: ERKO: 136.72 ± 19.21 mm−3 and WT: 68.73 ± 19.21 mm−3, p = 0.051). Significant group differences in DA were abolished when circulating fasting glucose was included as a covariate (without glucose: ERKO: 0.263 ± 0.029 and WT: 0.373 ± 0.027, p = 0.021; with glucose: ERKO: 0.282 ± 0.034 and WT: 0.358 ± 0.030, p = 0.172). In the lumbar vertebrae, significant group differences remained in BV/TV (without glucose: ERKO: 0.334 ± 0.013 and WT: 0.245 ± 0.013, p = 0.001; with glucose: ERKO: 0.325 ± 0.014 and WT: 0.253 ± 0.014, p = 0.011), Tb.N (without glucose: ERKO: 5.616 ± 0.137 mm−1 and WT: 3.891 ± 0.137 mm−1, p = 0.001; with glucose: ERKO: 5.603 ± 0.165 mm−1 and WT: 3.904 ± 0.165 mm−1, p = 0.001), and Tb.Sp (without glucose: ERKO: 0.124 ± 0.005 mm and WT: 0.197 ± 0.005, p = 0.001; with glucose: ERKO: 0.125 ± 0.006 mm and WT: 0.195 ± 0.006, p = 0.001). There were no significant relationships between circulating estradiol concentrations, fasting insulin concentrations, or percentage Sost+ osteocytes and other outcomes.
Discussion
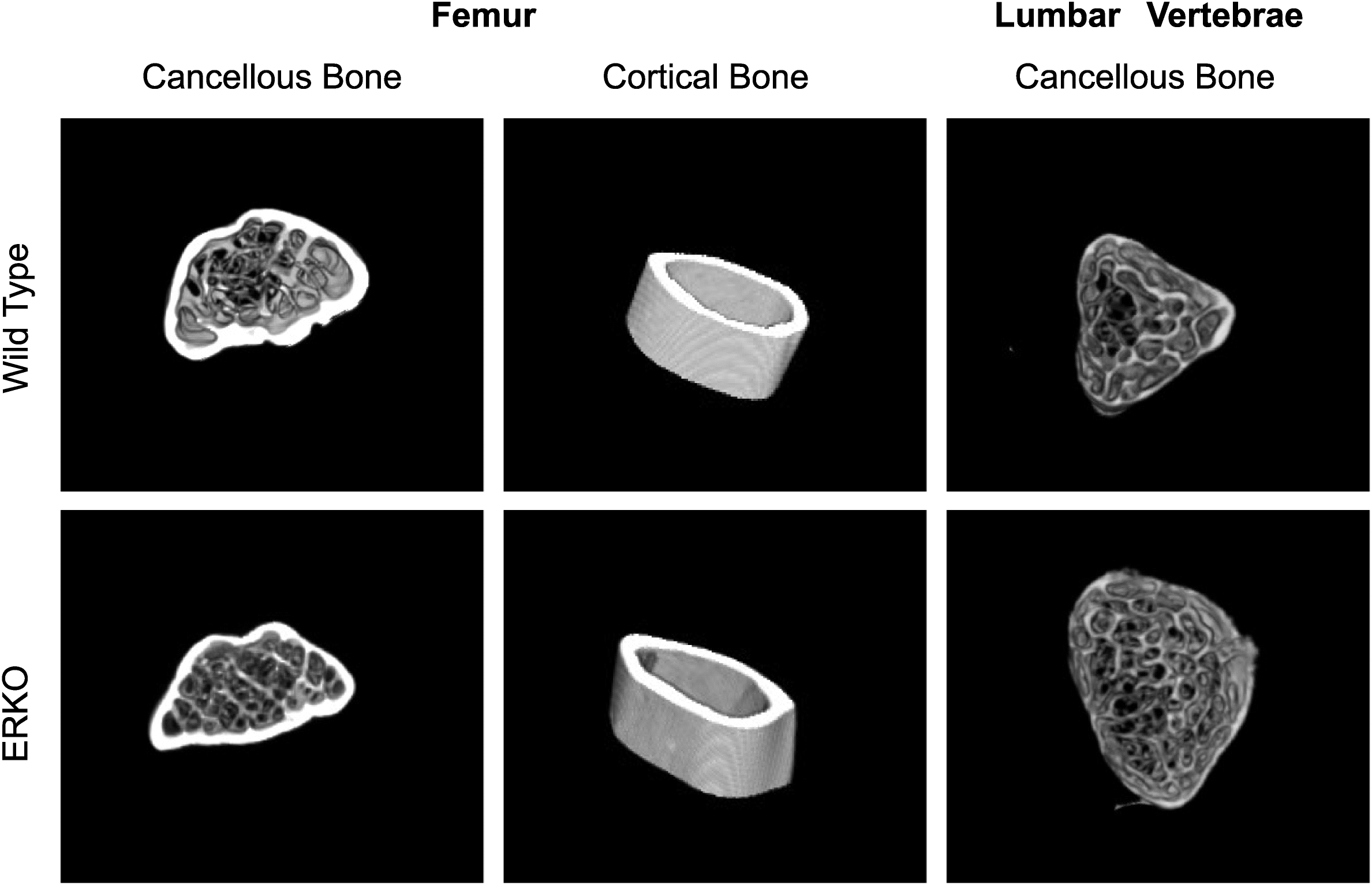
In this study, we showed that ERKO had differential effects on cancellous and cortical bone in aged male mice. ERKO animals showed changes in cancellous bone microarchitecture of the femoral distal metaphysis and lumbar vertebrae, which others have shown to be associated with increased fracture resistance (
Ebbesen et al. 1999;
Oxlund et al. 2001). By contrast, ERKO resulted in detrimental changes in cortical bone geometry of the femoral diaphysis compared with WT counterparts. This is the first study to assess sclerostin expression in a male ERKO model. ERKO did not increase sclerostin expression in cancellous bone of the distal femoral metaphysis or the lumbar vertebrae; however, sclerostin expression trended towards an increase in cortical bone of the femoral diaphysis. Furthermore, the skeletal effects of ERKO were not attributable to differences in overall metabolic health between ERKO and WT, implying that the skeletal phenotype is primarily attributed to the ERKO.
The morphological changes seen in the cortical bone in this study are supported by previous studies (
Vidal et al. 2000;
Lindberg et al. 2001;
Callewaert et al. 2009). Estrogen and the estrogen receptors have significant, cell-specific roles in the development and maintenance of bone mass (reviewed in
Khosla et al. 2012;
Khalid and Krum 2016), which directly influence bone remodeling. Estrogen blocks osteocyte and osteoblast apoptosis, induces osteoblast differentiation, increases osteoclast apoptosis, and reduces osteoclast differentiation through a direct suppression of receptor activator of NFκB ligand (RANKL) expression (
Syed and Khosla 2005;
Khosla et al. 2012). Estrogen indirectly reduces osteoclast differentiation through increased expression of osteoprotegerin, a decoy receptor for RANKL (
Shevde et al. 2000;
Bord et al. 2003). ERα specifically is required for the maintenance of cortical bone mass, as we can see in cell-specific ERα knockouts. When ERα was deleted from osteoblast precursors, femoral BMD and cortical thickness were reduced compared with WT animals, indicating that ERα controls cortical bone formation through actions on progenitor cells (
Almeida et al. 2013). This agrees with our results, since we only saw detrimental changes in cortical geometry and not in trabecular microarchitecture of the femur or vertebrae. However, when ERα was deleted from mature osteocytes only, trabecular bone volume of the lumbar vertebrae decreased, which is in contrast with our results (
Windahl et al. 2013). This is most likely due to the difference in cell-type; the deletion of ERα in just the osteocyte possibly produces a small enough effect on estrogen signaling that ERβ is not required to compensate as it often does in a whole-body model, though further studies in this area are needed.
As expected in a global knockout model, the improvements in vertebral trabecular microarchitecture were consistent with those observed in the femur and support our original hypothesis. The improvements we saw in trabecular microarchitecture of the femur are also consistent with previous studies done in younger male ERKO mice (
Lindberg et al. 2001;
Callewaert et al. 2009). These improvements can be explained by the greater presence of ERβ in cancellous bone where ERβ and ERα appear to have similar actions and both play a role in maintaining total bone mass (
Khalid and Krum 2016). However, one characteristic in our study that did not match previous studies is the lack of differences in femoral length. This could be in part due to the age of our animals compared with other studies, as mice do not fully close their epiphyseal plates and slowly continue longitudinal growth after sexual maturity (
Kilborn et al. 2002;
Jilka 2013).
Another possible cellular action of estrogen is the downregulation of sclerostin (
Kim et al. 2015b), which would also directly affect bone remodeling. In women, estrogen treatment decreased sclerostin mRNA concentrations in bone biopsy samples (
Fujita et al. 2014), but here we were the first to explore how a decrease in ERα could affect sclerostin expression in a male model. We hypothesized that, similar to previous female rodent models (
Kim et al. 2012;
Jia et al. 2014), the reduction in estrogen signaling would increase osteocyte sclerostin expression in male ERKO mice, as measured by immunohistochemistry. We observed increased osteocyte sclerostin expression in cortical bone in the ERKO animals that approached statistical significance (
p = 0.058), supporting the hypothesis that ERα plays role in the control of sclerostin expression. Interestingly, we only saw this change in the cortical bone, which directly correlated with the morphological effects also seen in the cortical bone. Therefore, we propose that downregulation of sclerostin is an important cellular action of estrogen in the overall control of bone remodeling and bone mass maintenance in cortical bone, and further studies are warranted.
Bone mass declines with aging, due to an imbalance in bone formation and resorption that favors increased bone loss (
Chan and Duque 2002;
Khosla 2013). In addition, serum concentrations of sclerostin increase with age in humans (
Khosla 2013;
Roforth et al. 2014;
Hay et al. 2016), although serum concentrations of sclerostin are not always reflective of sclerostin expression in the bone (
Delgado-Calle et al. 2017). For instance, bone needle biopsies of the iliac crest showed no difference in bone levels of sclerostin mRNA between young and old women, despite an increase in circulating sclerostin with age (
Roforth et al. 2014). However, in rodent models, there is a distinct increase in sclerostin as the animals age, whether measured by immunohistochemistry (
Thompson et al. 2016) or protein and gene expression (
Ota et al. 2013). Since the present study used an aged rodent model, it is possible that differences caused by ERα knockout were obscured by age-related increases in sclerostin (
Ota et al. 2013;
Thompson et al. 2016). Further studies are warranted to fully explore the importance of ERα in osteocyte sclerostin expression throughout the lifespan.
In addition to direct ERα-mediated effects on the bone, decreased ERα expression is associated with increased body weight (
Callewaert et al. 2009) and metabolic dysfunction, including insulin resistance (
Faulds et al. 2012) and type 2 diabetes (
Bryzgalova et al. 2006). These metabolic health concerns are associated with decreased bone quality (
Starup-Linde and Vestergaard 2016) and an increased risk of fracture (
Janghorbani et al. 2007;
Merlotti et al. 2010;
Compston 2013). In this study, ERKO mice were metabolically unhealthy, characterized by increased body fat percentage, glucose intolerance, liver steatosis, and increased fasting glucose and triglyceride concentrations (
Winn et al. 2018). We observed significant correlations between fasting glucose concentrations and trabecular microarchitecture outcomes, such as Tb.Sp, Tb.N, Tb.Th, BV/TV, DA, and Conn.D in both the femoral metaphysis and the lumbar vertebrae. Thus, to determine if the improvements in trabecular microarchitecture seen in the ERKO animals could be partly due to differences in glucose levels, we tested group differences with fasting glucose as a covariate. After accounting for differences in fasting glucose, the effect of ERKO on Tb.Sp, Tb.N, and Tb.Th remained, implying a direct effect of the loss of ERα activity on trabecular microarchitecture in the femur and vertebrae.
It is important to note that ERKO does not exactly mimic estrogen deficiency, given that estrogen signaling may occur via ERβ and there are ligand-independent effects of the ERα receptor (
Manolagas et al. 2013). In addition, female ERKO mice tend to have higher circulating estrogen levels (
Vico and Vanacker 2010), which could overemphasize the role of ERβ. However, in our study there were no differences in circulating estradiol between groups, which corroborates other studies done with male ERKO animals (
Nanjappa et al. 2018;
Winn et al. 2018). Another important note is that the knockout model used in this study is not a complete gene knockout, as it is achieved by splicing the neo cassette rather than removal of the full gene. In this and previous studies, this method has shown to be an effective knockout model, in that the interruption of the gene reduces estrogen receptor expression to levels undetectable by western blot (
Lubahn et al. 1993;
Iafrati et al. 1997). In addition, previous studies have shown that this knockout model has significantly reduced estrogen receptor activity, which manifests as significant phenotypic differences that can be attributed to the difference in the estrogen receptor gene (
Lubahn et al. 1993;
Eddy et al. 1996;
Heine et al. 2000).
One limitation of this study was that these mice were global ERKO mice, which did not allow for the distinction between osteocyte-, osteoblast-, or osteoclast-specific actions. Other studies have aimed to elucidate these cell-specific actions (reviewed in
Khalid and Krum (2016)), but none of them have looked at sclerostin expression, which makes this study novel. Another limitation was the lack of biomechanical strength data. While detrimental effects on cortical strength can be inferred, based on previous literature correlating a loss of cortical mass and thickness with a loss of biomechanical strength (
Ammann and Rizzoli 2003), we did not have the ability to test to biomechanical strength due to previous cracks and fractures that were revealed in the μCT analysis. Biomechanical strength can also be effected by the material properties of the bone, such as mineral composition and heterogeneity, collage composition and amount of crosslinking, and crystallinity of the material (
Bala and Seeman 2015;
Unal et al. 2018). While we saw no differences in mineral or collagen composition, the effects of ERα on other material properties are worth exploring.